Diagnosis
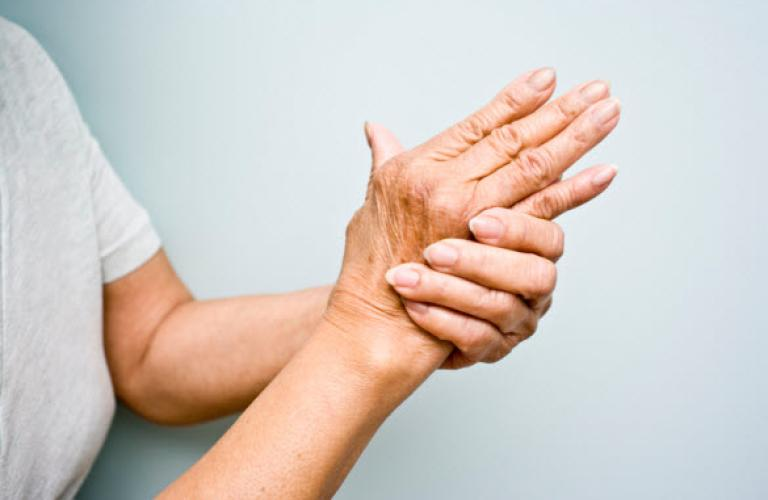
In its early stages, rheumatoid arthritis can be hard to diagnose since the early signs and symptoms resemble those of many other diseases. To validate the diagnosis, there is no single blood test or physical finding.
Your doctor will check the joints for swelling, redness and warmth during the physical exam. He or she will measure your reflexes and muscle strength as well.
Blood tests
People with rheumatoid arthritis also have an elevated rate of erythrocyte (ESR) or C-reactive protein (CRP) sedimentation, which may imply an inflammatory process in the body. Rheumatoid factor and anti-cyclic citrullinated peptide (anti-CCP) antibodies are looked for in other common blood tests.
Imaging tests
To help monitor the progression of rheumatoid arthritis in your joints over time, your doctor can prescribe X-rays. Your doctor will help determine the seriousness of the disease in your body with MRI and ultrasound tests.
Treatment
No Rheumatoid arthritis treatment has been discovered yet. However, clinical trials suggest that when therapy starts early with medications known as disease-modifying antirheumatic drugs, remission of symptoms is more likely (DMARDs).
Medications
Your doctor’s suggested types of drugs would depend on the severity of your symptoms and how long you have had rheumatoid arthritis.
- Nonsteroidal anti-inflammatory drugs (NSAIDs) can alleviate discomfort and decrease inflammation. Ibuprofen (Advil, Motrin IB) and naproxen sodium provide over-the-counter NSAIDs (Aleve). By prescription, stronger NSAIDs are available. Stomach irritation, heart attacks and kidney damage can be side effects.
- Corticosteroid drugs, such as prednisone minimize inflammation and discomfort and slow joint deterioration. Thinning of bones, weight gain and diabetes can be side effects. To alleviate acute symptoms, doctors frequently prescribe a corticosteroid, to eventually taper off the drug.
Disease-modifying antirheumatic medicine (DMARDs). These medications can delay the progression of rheumatoid arthritis and prevent permanent damage to the joints and other tissues. Popular DMARDs include methotrexate (Trexall, Otrexup, others), hydroxychloroquine (Plaquenil), leflunomide (Arava), and sulfasalazine (Azulfidine).
Surgery
You and your doctor can recommend surgery to fix damaged joints if medications fail to prevent or delay joint damage. Surgery could help to restore the ability to use the joint. It can also decrease pain and enhance function. One or more of the following procedures may require rheumatoid arthritis surgery:
- Synovectomy. Synovectomy Surgery may be done on the knees, elbows, ankles, fingers and hips to extract the inflamed lining of the joint (synovium).
- Tendon repair. Inflammation and joint damage can cause loosening or rupture of the tendons around your joint. Your surgeon can repair the tendons around your joint.
- Joint fusion. It may be advised to surgically fuse a joint to stabilize or realign a joint and for pain relief when a joint replacement is not an option.
- Total joint replacement. Your surgeon removes the weakened parts of your joint during joint replacement surgery and installs a prosthesis made of metal and plastic.
Surgery carries a risk of discomfort, infection and bleeding. Discuss the advantages and risks with your doctor before taking that step, if you experience discomfort and joint pain in knees, make sure to get the right medical attention.