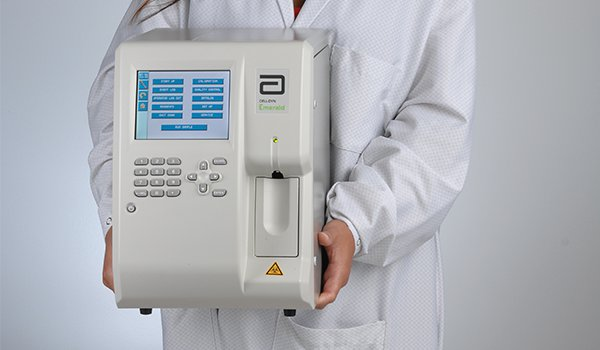
What is a Hematology Analyzer?
Hematology analyzers are used to quickly and accurately count and identify blood cells. Laboratory staff counted each solitary blood cell under a microscope in the 1950s. This was succeeded by Wallace H. Coulter’s first, extremely rudimentary hematology analyzer, which was tedious and inconsistent. Coulter’s Principle was used by the first hematology analyzers (see Coulter counter). They have, however, grown to include a wide range of procedures.
Blood samples are tested using hematology analyzers. White blood cell counts, complete blood cell counts, reticulocyte analysis, and related tests are all done using them in the medical laboratory.
Hematology analyzers is available for humans as well as animals blood analysis, making them helpful for veterinarians, zoos, and research facilities. Closed vial testing and open sampling testing are two features that differ from one hematological analyzer to the next.
The user can select the type of testing they want on some hematological analyzers. Other factors to consider in a hematology analyzer include the sample size required, the kind and amount of testing modes, the speed with which results are accessible, automated flagging of findings that are outside of the normal range, and the maximum number of test results it can handle.
What is a Hematology Stain?
Clinical and medical cytology research requires hematology stains and reagents. Staining makes difficult-to-see blood, bone marrow, and lymphatic system components visible and identifiable. The Wright, Giesma, and Leishman formulas function well on prepared blood smears, whether manually or machine processed.
All hematology stains are intended to act quickly for the most accurate results when working with time-sensitive samples. In hematology, Romanowsky stain solutions are utilized. Methylene blue, oxidative derivatives of methylene blue (Azure A, Azure B, Azure C, and Thionin), and eosin dyes make up these pigments. When used alone, Giemsa does not sufficiently stain the cytoplasms of red blood cells, platelets, or white blood cells.
Components of Hematology Stain:
- Routine hematologic stains:
Blood smears are stained using Romanowsky type dyes, such as a modified Wright’s stain (used at Cornell University’s Clinical Pathology Laboratory), and fast stains, such as Diff-quik®. Acidic (red) and basic (blue) dyes are used in these stains. Nuclei and RNA in red blood cells (RBC) show blue in smears, whereas hemoglobin in RBCs color red.
- Reticulocytes:
Reticulocytes are immature anucleate RBCs whose cytoplasmic RNA has been precipitated with a supravital dye (e.g. new methylene blue) or stained with a fluorescent dye (e.g. thiazole orange) for laser detection. Reticulocytes are recognised and counted at Cornell by their absorption of Oxazine-750, a nucleic acid-binding dye. These procedures are used to calculate the reticulocyte percentage, which is the number of immature anucleate RBC in the blood (of all RBC).
This measurement is only performed on dogs and cats on a regular basis. Reticulocytes are divided into two categories based on the quantity of RNA in their cytoplasm: aggregate and punctate (as seen in a new methylene blue-stained smear).
Types of Hematology Analyzer:
- 3-Part Differential Cell Counter
The size and volume of a cell are determined using Coulter’s Principle using a three-part differential cell counter. In a container that also holds a smaller container, the sample is lysed and dissolved in an electrolyte solution. Two pumps go to and from the smaller container’s solution, one generating a vacuum and the other refilling the lost solution. A tiny opening (an orifice) is located towards the bottom of the smaller container. Two electrodes are used to implement Coulter’s concept. The internal electrode is located within the smaller container, whereas the external electrode is located outside the smaller container but within the electrolyte/sample solution.
The sample cells generate electrical resistance to the current as it travels through the aperture as the vacuum drags them through the opening. This resistance is recorded, measured, amplified, and processed before being translated as a histogram by the computer. The three-part analyzer can distinguish between three distinct types of WBCs: neutrophils, lymphocytes, and monocytes.
- 5-Part Differential Cell Counter
To determine the granularity, diameter, and inner complexity of the cells, this type of hematology analyzer uses both Coulter’s Principle and flow cytometry. The cells are passed through an aperture one at a time utilizing hydrodynamic focusing. A laser is aimed at them during this process, and the dispersed light is measured from numerous angles. The absorbance is also taken into account. The intensity of the dispersed light and the amount of absorption can be used to identify the cell.
All WBC kinds may be distinguished using a 5-part cell counter (neutrophils, lymphocytes, basophils, eosinophils, and monocytes). 5-part analyzers cost more than 3-part analyzers, but they give more detailed information about the sample. Specific duties, such as allergy testing, necessitate the use of a five-part differential analysis. The 3-part analyzer, on the other hand, can handle most medical jobs.
Uses of Hematology Analyzer:
A complete blood count (CBC), which is frequently the first test ordered by physicians to establish a patient’s overall health state, is performed using hematology analyzers. Red blood cell (RBC), white blood cell (WBC), hemoglobin, and platelet counts, as well as hematocrit levels, are all included in a full blood count.
- The breadth of the RBC distribution
- The volume of the average corpuscle
- Hemoglobin concentration in the blood
- Concentrations of mean corpuscular hemoglobin
- The percentage and the absolute value of the WBC differential count
- The breadth of the platelet dispersion
- The average amount of platelets
- The platelet cell ratio is high.
- Criteria for platelets
Conclusion
Hematology analyzers are specialized equipment that counts the amount of white and red blood cells, platelets, hemoglobin, and haematocrit levels in a blood sample. Many hematologic illnesses can be diagnosed based on the findings of certain blood tests. Anemia, diabetes, autoimmune deficiencies, infections, and malignancies can all be detected by blood analysis. Genetic information, infections, and organ shortages can all be revealed.